Gender equality

By identifying and removing barriers to access and appropriate antibiotic use for migrant and refugee communities, health inequities and drug-resistance can be reduced nationally and globally.
Background:
Migrant and refugee communities often face heightened infection risks. They can also face limited access to formal health systems and additional legal, financial, and social barriers to care. These barriers increase reliance on informal or inappropriate antibiotic use. Addressing these gaps is essential not only to reducing health inequities, but also to strengthen national and global efforts to contain resistance.
What We Did:
In 2024, researchers at GSL conducted a global rapid scoping review to collect evidence of barriers to access and appropriate use of antibiotics among migrants and refugees. This research includes work completed with the World Health Organization as part of the Global Evidence Review on Health and Migration (GEHM) series.
Key Findings
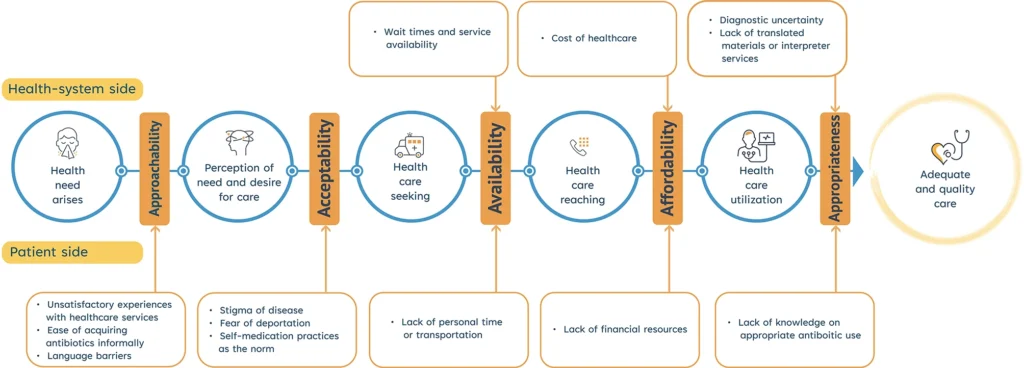
- Migrants and refugees experience barriers along the continuum of care from both the patient and health-system side, influencing access to quality-assured and appropriate antibiotics.
- Structural and social factors, like language barriers, fear of deportation, discrimination, long waiting times, limited transportation, and previous negative healthcare experiences, reduce trust in formal services, increasing reliance informal antibiotic use.
- Health system constraints, such as lack of insurance coverage, diagnostic uncertainty, limited availability of translated services, and substandard medicines, further constrain access to appropriate treatment and contribute to incorrect use of antibiotics.
- The study proposes global policy recommendations such as including refugees and migrants into WHO’s Global Action Plan on AMR to promote an equity-focused framework for coordinated action.
- National policy recommendations from this study include expanding language support, culturally tailored health education, and health literacy programs to promote access to appropriate antibiotic use.
Outputs
This global rapid scoping review, published in BMC Globalization and Health, collects evidence on how systematic, social and financial barriers play a role in antibiotic access and use among migrant and refugee populations.
The fourth report of the Global Evidence Review on Health and Migration (GEHM) series synthesizes available evidence on access to essential antibiotics in refugee and migrant populations. The report captures evidence across four themes related to antibiotic access and use: access, appropriate use, barriers to access and use, and interventions to improve access and use.
This visual resource highlights how structural, social, and health system barriers shape antibiotic access and use among migrant and refugee populations.

GSL researchers lead fourth report of World Health Organization’s Global Evidence Review on Health and Migration
On September 19, 2022, the WHO published the fourth report in the Global Evidence Review on Health and Migration (GEHM) series with a focus on Antimicrobial Resistance.

Policy Advisor for the AMR Policy Accelerator Attends CPHA 2024 Conference
Suzanne Naro, Policy Advisor for the AMR Policy Accelerator, addressed the challenges faced by migrant and refugee communities in accessing antibiotics during her presentation at the Canadian Public Health Association (CPHA) 2024 conference.

When promises aren’t enough: Improving access to antimicrobials amidst global crises
As the world faces rising levels of antimicrobial resistance (AMR), the disparities in access to essential antimicrobials have become more apparent, particularly in low- and middle-income countries. At the same time, numerous regions grapple with conflict, and it is critical to understand how the disruption of health systems and the displacement of populations, with a disproportionate percentage being women and children, further impede global action on AMR.
York U study warns gaps in antibiotic access pose global health threat
Migrants and refugees face an increased risk of unsafe antibiotic use and resistance which poses a significant global health threat, according to new research led by York University.
